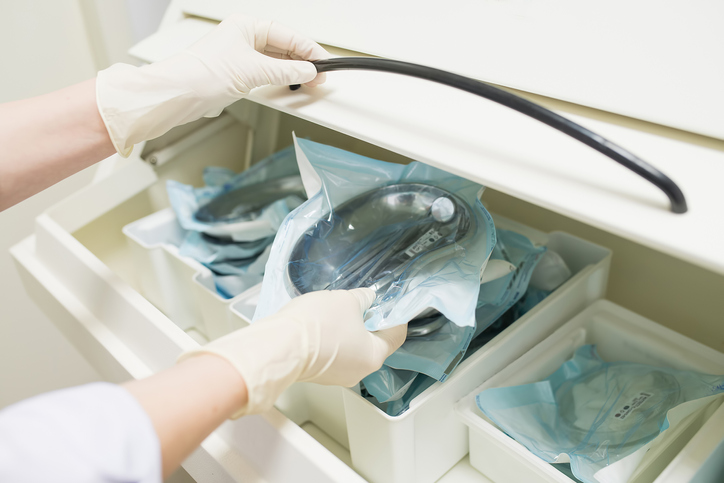
Perhaps nothing has proven the indispensable value of commercial sterilizers more than the devastating worldwide COVID-19 pandemic. Without the highly effective and efficient commercial sterilizer ethylene oxide (EtO), we would not have been able to rely on lifesaving sterilized medical equipment and supplies – such as cotton swabs for nasal-swab testing, masks, ventilators, and thermometers – to get us through the past four years. Moreover, maintaining basic hospital functionality and everyday healthcare needs outside of the pandemic requires sterile equipment and supplies simply for civilization as we know it to persevere in a healthy, sustainable way. Put simply: EtO has arguably saved millions, if not billions, of lives.
Increasing knowledge about the potential hazards of EtO-sterilizing-facility emissions to fence-line communities (extensively covered by ELM here, here and here), much more stringent regulations of EtO’s use (covered by ELM here, as well as here, in which we break down the long-awaited regulations in detail), and basic logistical and supply limitations of providing the entire world with a single sterilizer (covered by ELM here), however, highlight the necessity of developing some viable alternatives to EtO.
As part of its push to develop alternatives to EtO and associated sterilizing innovations (covered by ELM here), on January 8, 2024 the U.S. Food and Drug Administration recognized vaporized hydrogen peroxide (VHP) as a Category-A sterilization method. According to the FDA, “Methods with a long history of safe and effective use on medical devices are considered Established Category A sterilization methods and include moist heat, dry heat, EtO and radiation.”
This approval is based on the hope that it will result in less dependence on EtO as a sterilizer for medical devices, which has been a specific goal set by the FDA while the U.S. Environmental Protection Agency simultaneously worked on stricter, recently disclosed EtO regulations. More specifically, the FDA’s January 8 announcement explained, “This update will facilitate broader adoption of VHP as a sterilization method for the medical device industry, is part of the agency’s multi-pronged approach to reducing the use of [EtO] where possible and further supports the agency’s efforts to advance medical device supply chain resiliency.” Furthermore, this approval is expected to boost interest in developing EtO alternatives in that it shows that progress is indeed possible. In fact, industry analysts have predicted aggressive growth in the commercial sterilizer industry, particularly given intense regulatory focus on EtO and the trauma of overextended EtO supply chains.
Given recent winter-weather-related events, this EtO news could not be timelier. With nearly all the United States experiencing an Arctic blast this week, the EtO industry and supply chain (the precariousness of which ELM reported on here) has not escaped impact. Much of the EtO industry is based in Texas, some parts of which reported temperatures reaching below freezing. This highly unusual weather for the Lone Star State resulted in significant interruptions for EtO production and use, such as closing Port Houston’s terminals as a precaution against having to transport chemicals on icy highways; process upsets; rate reductions; and partial and full EtO plant shutdowns at major chemical companies.
Consequently, having more than one commercial sterilizer option produced in more than a single primary region of the U.S. increasingly appears to be the only way to battle against what seems to be an ever-growing pile-up of historic force majeure calamities such as once-in-a-century pandemics or dramatic climate events.